We all know someone living with diabetes, but what most people don’t know is that Hispanic adults are 70% more likely than their non-Hispanic white counterparts to be diagnosed with diabetes by a physician, according to the U.S. Department of Health and Human Services. Diabetes can be a dangerous and even deadly chronic condition and understanding why it disproportionately impacts the Hispanic community is key to eradicating health disparities.
What is Diabetes?
Diabetes is a chronic disease that affects how your body turns food into energy. Essentially, the pancreas doesn’t make insulin or makes very little insulin. Without insulin, blood sugar can’t get into cells, and it builds up in the bloodstream. High blood sugar is damaging to the body and causes many of the symptoms and complications of diabetes. There are three main types of diabetes: type 1, type 2, and gestational diabetes (diabetes while pregnant). While the different types of diabetes are similar in some ways, it is important to understand that they are distinct regarding how they develop, who they affect, and how they must be managed.
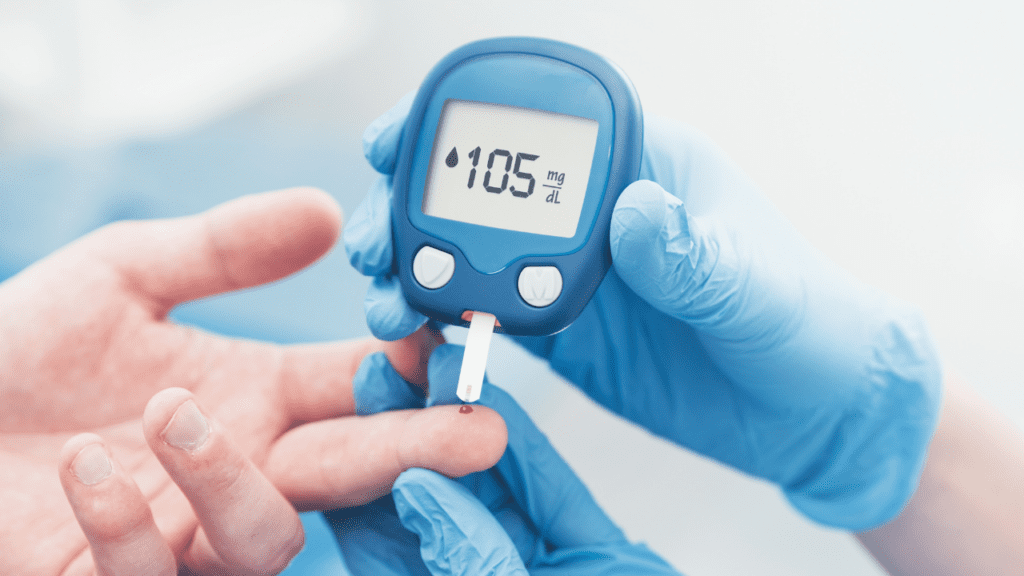
Type 1 diabetes is usually genetic and most often develops in children, teens, and young adults, but it can happen at any age. Currently, no one knows how to prevent type 1 diabetes, but it can be treated successfully by managing blood sugar levels, eating healthy, and getting regular checkups. Type 1 diabetes is less common than type 2—about 5-10% of people with diabetes have type 1. However, its incidence is increasing across the country, especially among Hispanic youth.
Type 2 Diabetes
Type 2 diabetes is distinct from type 1 primarily in that it is not genetic, but rather develops over time and is mainly lifestyle related. The CDC reports that Hispanics living in the U.S. are 17% more likely to have type 2 diabetes than non-Hispanic white people. For those with Puerto Rican or Mexican heritage, the risk of developing type 2 diabetes can be twice as high, compared to those with South American heritage.

Over their lifetime, Hispanic or Latino adults have a 50% chance of developing type 2 diabetes, and they’re more likely to develop it at a younger age. Diabetes complications also hit harder: Hispanic populations have higher rates of diabetes-related kidney failure, vision loss, and mortality rates.
Investigating Diabetes’ Disproportionate Impact on Latino Communities
We know that diabetes disproportionately affects Hispanic communities. But why? While further studies are needed to investigate this health disparity, researchers have been able to point to several potential factors.
Many of the increased risk factors for diabetes among Hispanics stem from socioeconomic status. 23% of Hispanics in the U.S. live below the poverty line, which often correlates to lower health literacy rates, higher uninsured rates, lack of access to regular healthcare, and other environmental hazards.
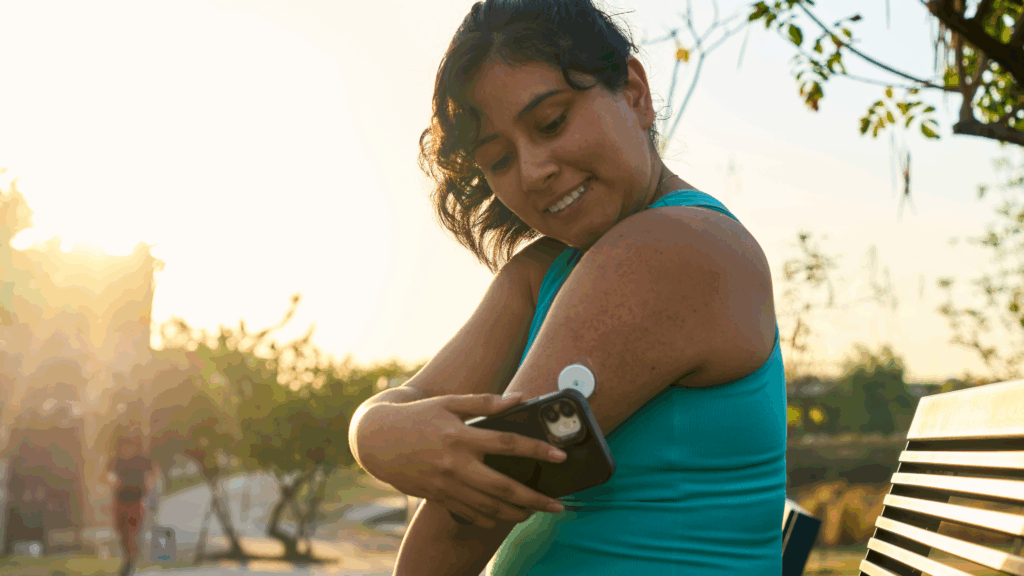
This also contributes to high rates of food insecurity, which affects 22.4% of Hispanic households, according to the USDA. Latino households spend a third of their income on food, a majority of which is calorie dense, low in fiber, and high in fat, sodium, and carbohydrates. High carbohydrate intake can cause blood sugar levels to rise and foods high in fat contribute to obesity, a leading risk factor for type 2 diabetes.
Food as Culture in Hispanic Communities
Addressing nutrition is an essential element of diabetes prevention within the Latino community, especially given that obesity is more prevalent among Hispanic youth (21.9%) compared to their non-Hispanic white counterparts (14.7%).
However, this can be a complex task, as it is important to acknowledge relevant cultural context, such as Latinos’ strong family connections, and meal-sharing as an important tradition. Food serves as a huge bond among Latino families and also a connection with their roots.

While having food in the spotlight of Latino family gatherings and in daily life is a beautiful piece of Hispanic heritage, most traditional Hispanic dishes tend to be high in fat, carbohydrates and calories. Also, family gatherings may involve social pressure to overeat, reports the CDC. For most Latinos, refusing to eat your mom or grandma´s dishes could be difficult or even considered disrespectful.
So, when a family member has to change what they eat to manage or prevent diabetes, it affects the whole family. This can be an opportunity for everyone to make healthy changes, which is especially important for kids. Hispanic and Latino children and teens are at higher risk for developing type 2 diabetes too and learning healthy eating habits early gives them the best chance to prevent it.
But there is a silver lining: it´s totally possible to enjoy tasty Hispanic food and stay a step ahead of diabetes. There are options to stay close to family roots, enjoy your favorite dish, and still eat diabetes-friendly too.
Preventing Diabetes While Eating Traditional Hispanic Dishes
Many foods in the Latino diet are naturally healthy, from black beans and avocados to fresh fruits and whole-grain corn. However, there are also many Latino dishes which are fried and prepared with processed ingredients, and those should be limited.
There are several ways to tweak favorite Hispanic dishes’ traditional recipes to make them more diabetes-friendly, including minor ingredient swaps, switching cooking methods (from fried to baked, for example), and adjusting portion sizes.

Here are some basic tips on good nutrition adapted from the Together 2 Goal® campaign to remember when meal planning:
- For protein sources, look for fresh seafood, lean poultry, and beans. Consider foods such as ceviche, a veggie black bean wrap, baked empanadas, or chicken fajitas/tortas.
- When preparing traditional dishes that have ground meat in the recipe, choose 93% lean ground turkey or ground sirloin beef when possible.
- When eating salsa, choose fresh salsa over store-bought. While the store brand may be low in calories, it usually has a high amount of salt.
- Swap white rice for brown. As a whole grain, brown rice has more nutrients. Consider cauliflower rice too!
- Try to keep the fat used when cooking to a minimum and avoid unhealthy fats like lard and butter. A little vegetable or olive oil or cooking spray are better options.
- Use healthy cooking methods like grilling, baking, steaming, or broiling.
- Choose dried beans when possible. They generally have less sodium than canned.
- Be aware of cheese portions. Cheese can be high in saturated fat and sodium. Look for reduced-fat cheeses when shopping.
- In dishes that call for sour cream, consider using nonfat Greek yogurt or nonfat plain yogurt instead. They have fewer calories and fat than sour cream but with a similar taste and texture.
The Need for Culturally Appropriate Diabetes Education
Creating healthy eating habits to prevent or manage diabetes while also maintaining strong ties to Hispanic food culture is certainly feasible. However, there is a huge gap when it comes to effective diabetes education for Latinos. While language disparities can be a barrier to care and adherence to prevention or treatment plans, native-language educational materials alone are not sufficient.
It is also vital to adapt to cultural values, traditions, and dynamics. In fact, when properly leveraged, Hispanic culture can actually improve diabetes outcomes. Studies have shown that the strong family support systems often observed in Latino cultures facilitated increased adherence to diabetes management plans.
And yet, culturally competent diabetes programs are scarce. While there are some examples of specific programs that we can point to and learn from, such as Joselin Diabetes Center’s Latinx Initiative, there is still a significant need for culturally sensitive diabetes education and management programs that consider diverse traditions and practices, while maintaining high-quality care.
Ultimately, this requires changes at both the clinical and organizational levels for health care institutions. Additionally, health literacy as a whole, whether taught in k-12 or in medical settings, needs to be modified to be inclusive of these cultural aspects.
Image source:
- Older Woman talking with the Doctor stock photo by FatCamera from Getty Images Signature
- Doctor Checking Blood Sugar Level with Glucometer by Proxima Studio
- insulin, diabetes, diabetic child. by burcu saritas from Getty Images
- Diabetic patient woman doing exercises. Continuous Glucose Monitor and active sugar diabetes lifestyle by Fabián Montaño from Fabian Montaño
- Old Mother and Adult Daughter Eating Cake at Home by Syda Productions
- Green Enchiladas Mexican Food with Guacamole by Lunamarina
- Man Holding a Glucose Monitoring Pen by halfpoint

